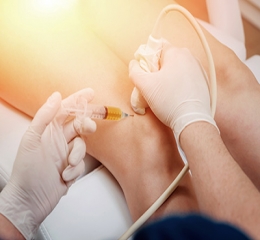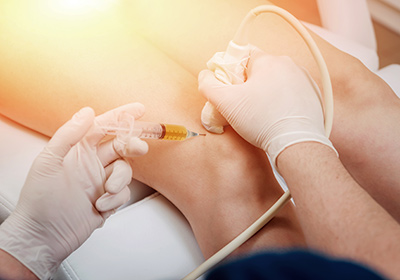
Patients often ask me about PRP. PRP stands for platelet rich plasma. It is a liquid that is obtained from a patients’ blood. The blood is drawn from a patient’s vein. A centrifuge is then used to separate out the parts of the blood. The main parts of blood include the red blood cells which carry oxygen, the white blood cells which monitor and address infection, platelets which help with healing and the plasma which carries proteins and other substances important for healing and regular bodily functions. In PRP, the red blood cells are removed. The platelets and plasma are retained. Depending on the potential site of injection, varying levels of white blood cells are removed.
PRP can be both pro-inflammatory (meaning it increases inflammation) or anti-inflammatory (meaning it decreases inflammation) depending on the formulation of the injection. Both formulations can be useful depending on if more inflammation or less inflammation is what the problem calls for. Much of this determination is based on the location and type of pathology being addressed.
The anti-inflammatory effects of PRP are most useful when dealing with arthritic and degenerative conditions. PRP has evidence in the treatment of arthritis. The strongest evidence is from a very high quality study out of Rush in Chicago. It is a randomized, prospective, double blind, controlled trial. They found that PRP is more effective at managing pain from knee osteoarthritis and improving function than injections of lubricating hyaluronic acid. I would consider an anti-inflammatory PRP injection for the treatment of knee arthritis, especially if I had tried cortisone (steroid) and hyaluronic acid without significant relief and was trying to avoid a knee replacement.
The second place that I would consider a PRP injection is in the treatment of an acute sprain or strain. The pro-inflammatory formulation of PRP is especially useful in this setting. The goal is to increase inflammation with the secondary effect of speeding healing time. To go down this pro-inflammatory road, the patient must make a conscious decision to avoid anti-inflammatory modalities including ice and NSAIDs (like ibuprofen and naproxen). These medications and modalities counteract the effect of the pro-inflammatory PRP. Specific locations that I would consider include an ankle sprain, patellar tendonitis, MCL sprain, and other ligament sprains/tendon strains.
PRP can be a useful adjunct to the other mainstays of orthopaedic treatment; medication, physical therapy, activity adjustments and R.I.C.E. PRP injections are generally not covered by insurance companies so patients (and the doctors who care for them) must be mindful of the financial side effect of the treatment; especially in cases where it used without significant scientific evidence. I would not consider PRP for myself for all orthopaedic maladies but I would certainly consider it to treat the two general problems mentioned above.
The content found herein is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read here.